Diabetic Foot Calluses: How to Treat Them- With the advent of smartphones and tablets, more and more people can access the Internet anytime. This has changed the way people communicate, interact and learn. When we say this, it does not mean that all mobile phones are the same. There are a few different types of mobile phones, and each one works slightly differently.
![Diabetic Foot Calluses: How to Treat Them 1 How to remove a callus from a diabetic foot? [Foot Corn & Callus Removal]](https://www.michiganfootdoctors.com/uploads/2021/09/Ball-of-the-foot-callus-1024x1021.jpg)
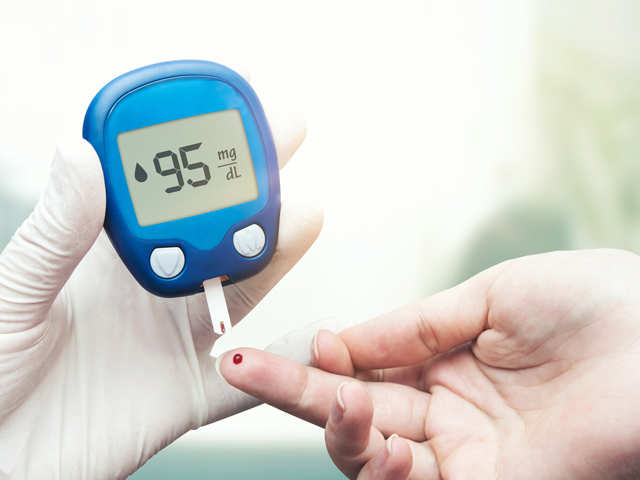
Diabetes is a disease that affects nearly 30 million people in the United States alone. A large percentage of people living with diabetes have foot complications. These include diabetic foot ulcers, which are painful and sometimes life-threatening.
Are you tired of taking drugs to treat your diabetic foot calluses? If so, you are not alone. In fact, according to a survey conducted by the National Institutes of Health, more than half of all people with diabetes are taking prescription drugs to treat their wounds.
Fortunately, there are other options for treating these painful wounds. This blog post will look at some natural alternatives to conventional diabetic foot care.
What is a diabetic foot callus?
Diabetic foot calluses are the body’s response to neuropathy, a nerve condition caused by long-term diabetes. They can range from small, flat lesions to large, painful areas of thickened skin.
They often occur on the bottom of the foot and are commonly found in people who have poor blood circulation in their feet. Some people with diabetes may have more calluses, while others may have fewer.
The best way to treat diabetic foot calluses is by combining regular wound care and medication.
Why do you need to remove the callus
Diabetic foot calluses are often painful and difficult to treat. They can be caused by walking on hard surfaces such as floors or sidewalks.
Foot calluses are typically formed from repeated pressure and friction over an extended period. When the callus is broken, it can lead to infection.
Calluses also cause nerve damage, which can cause pain. Additionally, they can prevent the foot from functioning properly.
How to remove diabetic foot callus
People with diabetes have a higher risk of developing a diabetic foot ulcer because the skin of their feet becomes thinner and more fragile due to poor circulation.
The ulcers are caused by minor damage to the skin, which can be aggravated by trauma or pressure. They usually occur on the bottom of the foot and are often seen on the toes, the heel, or the sides.
If you have a diabetic foot ulcer, you will need to take care of it immediately. The sooner you address the problem, the better.
There are several ways to treat diabetic foot ulcers. In the following article, I’ll show you how to get rid of diabetic foot ulcers using a home remedy.
Diabetic Foot Callus Removal
You might be wondering how to remove your calluses without medication. I have found that the best way is to massage the calluses using a massage cream. Doctors recommend this method for healing chronic wounds, which should work great for treating diabetic foot calluses.

Frequently Asked Questions(FAQs)
Q: What does it feel like when your foot gets a callus?
A: When my feet got a callus, it felt like there was a rock in my shoe. You are never really sure how big your foot will get until you look down at it. Many people don’t care what their feet look like, but I’m picky.
Q: How can you tell if you need to get your foot checked out?
A: If you feel a hard lump or pain under your skin, you should visit the doctor.
Q: How long does it take to heal?
A: It depends on the severity of the wound. I had two very large injuries. It took me about a week to get the wounds to close. It took me a couple of months to get the calluses to go away. It takes time for your body to heal itself.
Q: How long does it take for diabetic foot callus to form?
A: Most of us have this foot condition because we are not paying attention to our feet. We think it’s just dry skin. But it’s a sign of poor circulation. A lack of blood flow usually causes calluses. A blood vessel becomes engorged and constricted. When the callus forms, the area is not receiving enough blood flow, which causes the skin cells to harden. This is why it takes a while to develop a callus; you have to have time to fill in the area with healthy new skin cells.
Q: How can a person tell if they have diabetic foot callus?
A: A hard, thickening patch of skin on the bottom of your foot or lower leg is most likely a callus.
Q: What’s your story about your diabetic foot callus?
A: I got my first diabetic foot infection about two months ago, which had gotten bad. The big toe on my left foot was split open, and I wasn’t sure what to do. I went online and found someone who treated this with a chemical, and it healed quickly. I didn’t know what the chemical was, but I trusted him and am now healed.
Q: What do you recommend to help other diabetic patients avoid similar problems?
A: I would suggest to anyone with diabetes to go to the doctor and take care of their feet.
Myths About Diabetic Foot Calluses: How to Treat Them
1. Diabetic foot ulcer (DFU) does not heal by itself.
2. A simple wound cannot cure diabetes.
3. A diabetic wound should be treated with a diabetic dressing.
4. Diabetic foot calli are normal.
5. Diabetic foot calluses can not be treated by just changing their dressings.
6. Diabetic foot calluses are caused by poor blood supply.
7. Diabetes causes the foot to dry out and become brittle.
8. Diabetics do not like to walk and should not be allowed to walk on hard floors.
9. It is a normal response to trauma to the feet and heals quickly.
10. You should not try to remove it until it becomes a serious infection.
Conclusion
It is important to note that some of the information provided here may not apply to all patients.
This article will focus on how to prevent and treat the diabetic foot ulcer and callus. It will discuss the factors to consider in choosing a treatment option and how to manage your patient.
A diabetic foot ulcer can occur if the patient’s feet are not properly cared for. It is most commonly associated with diabetes, peripheral vascular disease, and peripheral neuropathy.
A diabetic foot ulcer may develop due to poor blood flow to the skin. This results in tissue breakdown and infection.
The first step in treating a diabetic foot ulcer is determining whether the condition is caused by peripheral vascular disease. If it is caused by peripheral vascular disease, the patient should be treated with a compression therapy device and a dressing such as a foam pad.
If it is caused by peripheral neuropathy, the patient should receive a therapeutic shoe and an orthotic that supports the heel.